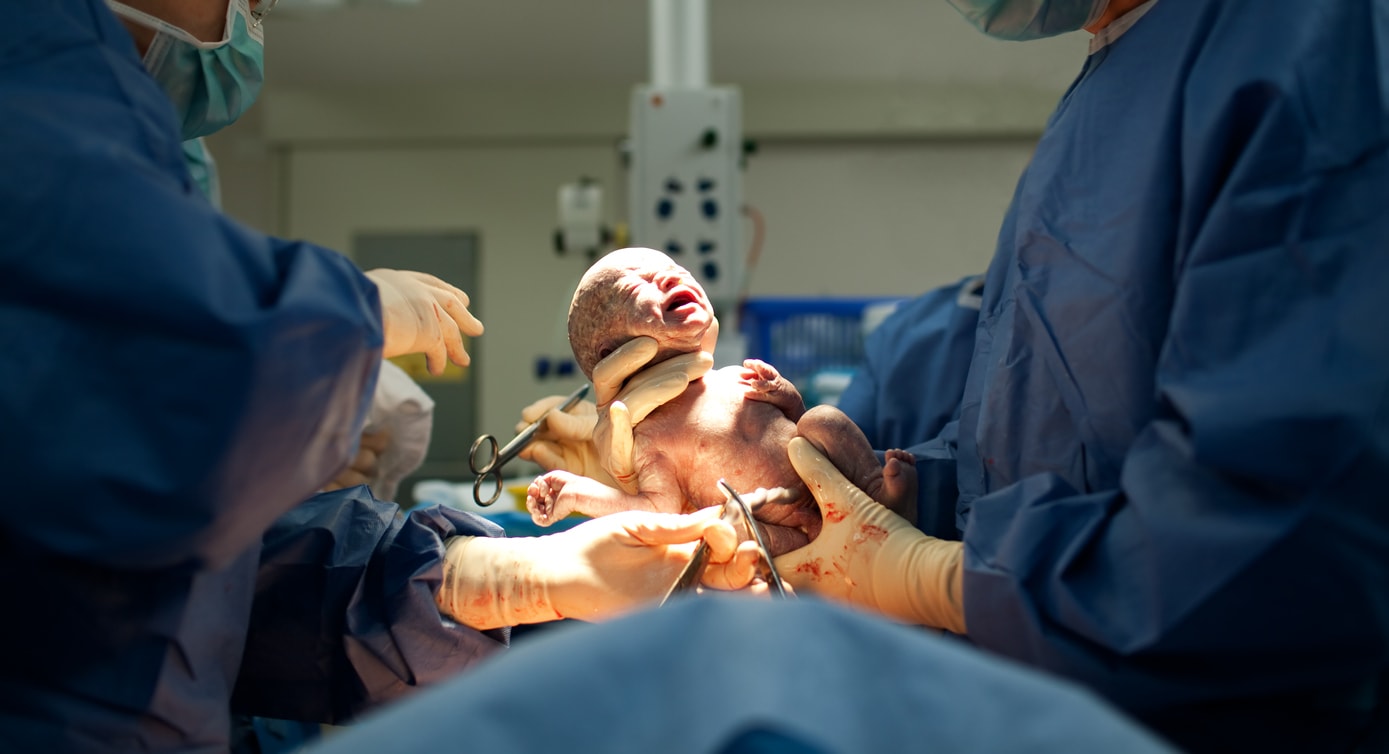
Pediatric patients with limited English proficiency (LEP) may face additional challenges when they present to an emergency room. However, researchers from Children’s Hospital of Philadelphia (CHOP) found that a multidisciplinary approach helped implement the services of interpreters earlier and significantly improved the identification of these patients to help them receive the care they need. The findings were published online by the journal Pediatrics.
Patients with LEP face a number of challenges, including an increased risk of adverse events due to potential medication error, as well prolonged or repeat visits to the emergency department. When treating children, the language needs of both the patient and the caregiver must be met, adding further challenges to delivering the best care possible.
Medical interpreters are vital to making sure patients with LEP receive proper treatment; however, many caregivers are unaware that this service is available to them. A review found only about 2.5% of patient encounters in the emergency department utilized an interpreter, but census data suggests that in CHOP’s region, roughly 10% of patients have at least one parent with LEP.
The data we had prior to this study suggested there was underrecognition of the language needs in our emergency department. We wanted to improve early identification of patients and caregivers who could benefit from an interpreter and make sure those services were properly tracked in health records so we could continue to meet their language needs.”
Katherine M. Gupta, MD, first study author, attending physician in the emergency department at CHOP
The research team identified areas that could help improve the emergency department workflow for patients with LEP and introduced a series of interventions to increase the identification of language needs and offer interpreters as needed. These processes included a screening question during nursing triage, an icon on the emergency department track board that helps communicate language needs to the emergency department staff and alerts for electronic health records.
After implementing these measures for six months, the team observed several noticeable improvements in identifying language needs in the emergency department. Identification rates for patients with LEP during the nursing triage increased from 60% to 77%, interpreter utilization increased from 77% to 86%, and proper documentation of interpreter use increased from 38% to 73%.
“By implementing the methods used in this study, we have an opportunity to obtain more reliable metrics on patients with LEP and investigate the true extent of language-based disparities in care,” said senior study author Joseph Zorc, MD, an attending physician in the Emergency Department and Director of Emergency Information Systems at CHOP. “Our staff has become keenly aware of the language needs during emergency department visits and there is growing interest in addressing LEP issues and investigating the feasibility of dedicated in-person interpreters specifically assigned to emergency department cases.”
Source:
Journal reference:
Gupta, K.M., et al. (2023) Improving Identification of Interpreter Need in the Pediatric Emergency Department. Pediatrics. doi.org/10.1542/peds.2022-057330.