If you have sharp abdominal pain, vaginal bleeding, or other unusual symptoms, then you may be experiencing an ectopic pregnancy. This requires immediate medical attention.
What makes an ectopic pregnancy confusing to diagnose is that sharp abdominal pains could also be normal. For example, round ligament pain is a cramp-like feeling in the lower abdominal area that affects 10% to 30% of pregnancies—and is totally harmless. That’s why it’s important to gather all the information and reach out for help if you’re worried.
Below is everything you need to know about ectopic pregnancies, including what to look for and how it is treated.
What is an ectopic pregnancy?
An ectopic pregnancy occurs when a fertilized egg implants outside the uterus, causing the embryo to grow outside the womb. This is a high-risk condition that always results in pregnancy loss, and it could lead to heavy bleeding or death for the pregnant person. Seek immediate medical attention if you think you have an ectopic pregnancy.
In more than 90% of ectopic pregnancies, the embryo grows in a fallopian tube, according to the American College of Obstetricians and Gynecologists (ACOG). If this growth causes the tube to rupture, it can cause life-threatening internal bleeding that requires immediate surgery.
Related: Overturning Roe v. Wade is about so much more than abortion
Ectopic pregnancies occur in 1.9% of reported pregnancies (or 1 out of every 50 pregnancies), according to the American Academy of Family Physicians, and is the number-one cause of pregnancy-related death in the first trimester.
What are the different types of ectopic pregnancies?
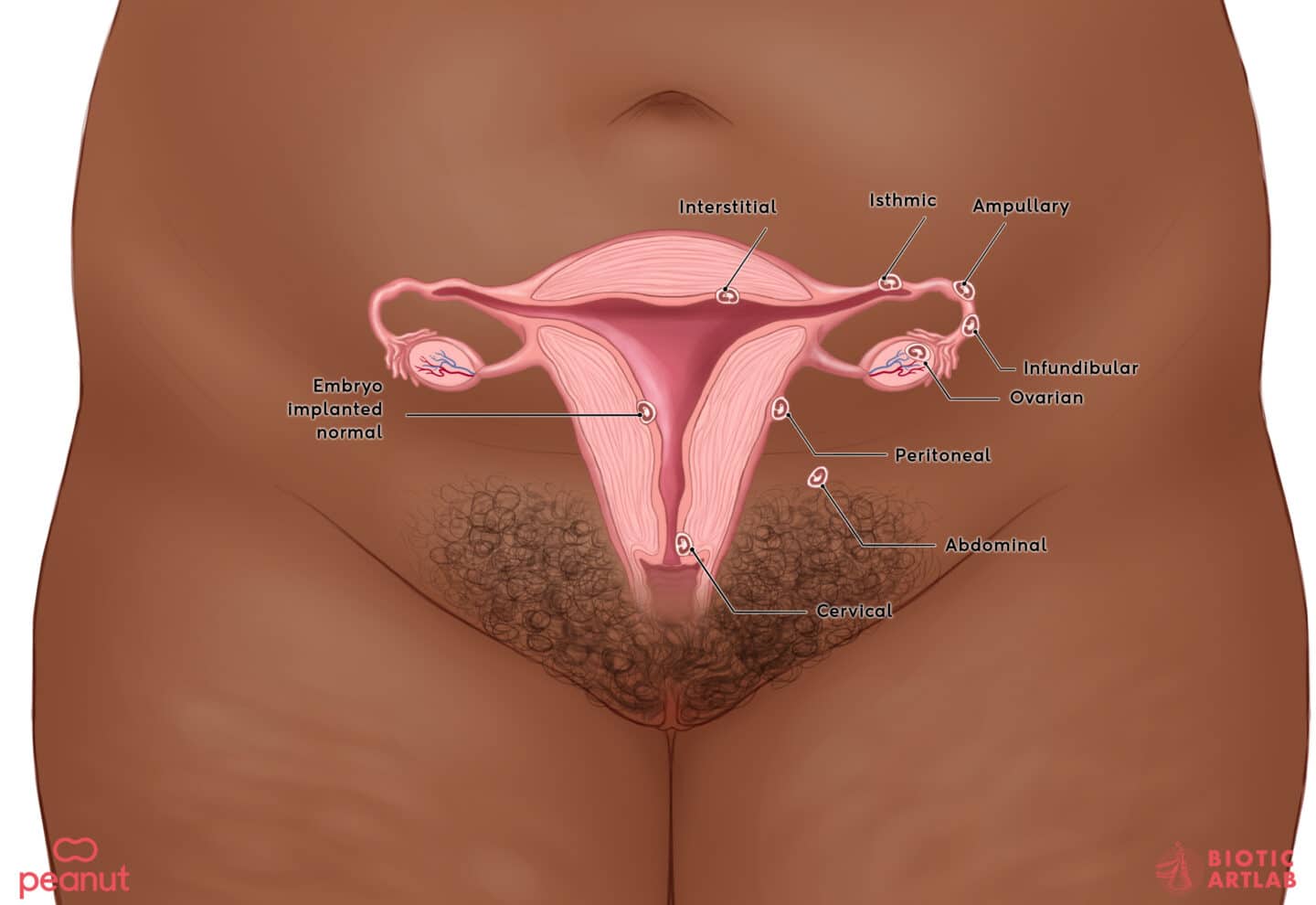
The most common site of an ectopic pregnancy is in the fallopian tube, which are the tubes connecting the ovaries and the uterus. This is called a tubal ectopic pregnancy.
Uncommon implantation sites of an ectopic pregnancy include:
- Cervix
- Interstitial segment of the fallopian tube
- Scar from a prior cesarean delivery
- Uterine myometrium
- Ovary
- Peritoneal cavity
A heterotopic pregnancy is a rare instance of an intrauterine and an extrauterine pregnancy, or two ectopic pregnancies, occurring simultaneously.
Symptoms
Ectopic pregnancies can be difficult to detect at first, because they share many of the same signs as a typical pregnancy, including a positive pregnancy test, a missed period, morning sickness and other symptoms.
Call your doctor if you experience these signs or symptoms of an ectopic pregnancy:
- Vaginal bleeding
- A faint or dizzy feeling, which can be caused by low blood pressure
- Pain in your lower back or shoulder
- Pain in your pelvic area, particularly if it’s on just one side. This pain can come and go, and it can change in intensity levels—from mild to sharp and stabbing
If the ectopic pregnancy continues to grow and leads to a ruptured fallopian tube (which can cause life-threatening internal bleeding), you may develop these symptoms:
- Sudden, severe pain in the abdomen or pelvis
- Shoulder pain
- Weakness, dizziness or fainting
If you have these symptoms, you should go to the emergency room immediately.
Diagnosis
To diagnose an ectopic pregnancy, your health provider may perform a pelvic exam or a transvaginal or transabdominal ultrasound to see where the embryo has implanted.
Or your provider may test your blood to measure the levels of pregnancy hormone human chorionic gonadotropin (hCG), which can rise more slowly in an ectopic pregnancy than an in intrauterine pregnancy or fall more slowly than is commonly seen in a miscarriage.
In some cases, your provider may also have to perform surgery to diagnose an ectopic pregnancy.
Treatment
An ectopic pregnancy cannot move or be transferred to the uterus, and it always requires immediate medical attention. The only place for a baby to safely grow is the uterus, so an embryo that grows outside the uterus can cause the place where it has been implanted to bleed heavily or burst, according to the March of Dimes.
ACOG says ectopic pregnancies are commonly treated with methotrexate, which stops cells from growing. The pregnancy will be absorbed by the body in 4 to 6 weeks, and you will be monitored to check for dropping hCG levels. (Note: You cannot use methotrexate if you are currently breastfeeding.)
Related: What now? How to get involved after the overturning of Roe v. Wade
Laparoscopic surgery may be necessary to treat an ectopic pregnancy. Typically, this is done through small cuts in the abdomen to remove the embryo from where it has implanted. In some cases, the entire fallopian tube may be removed in a tubal ectopic pregnancy.
Risk factors
An ectopic pregnancy could happen to anyone. According to ACOG, about one-half of all women who have an ectopic pregnancy do not have known risk factors. So, you should always monitor your symptoms before your first ultrasound to watch for anything unusual.
Here are a few risk factors that can make you more likely to experience an ectopic pregnancy:
- Previous ectopic pregnancy
- Prior fallopian tube surgery or a birth defect in the fallopian tube
- Scars in the pelvic area from previous pelvic or abdominal surgery
- Pelvic inflammatory disease
- Endometriosis
- Getting pregnant while using an intrauterine device (IUD) or after tubal litigation (getting your tubes tied)
- Cigarette smoking
- Being 35 years old or older
- A history of infertility
- Use of assisted reproductive technology, such as in vitro fertilization (IVF)
- Having more than one sex partner, which can put you at risk for a sexually transmitted infection (STI)
Can I get pregnant again after having an ectopic pregnancy?
Yes, you can get pregnant again after having an ectopic pregnancy. According to the March of Dimes, about 1 in 3 women (or 33%) who have had an ectopic pregnancy go on to have a healthy pregnancy. Keep in mind, if you’ve had a prior ectopic pregnancy, there is about a 3 in 20 (or 15%) chance you’ll have another. So, if you do get pregnant after an ectopic pregnancy, you should closely monitor your early pregnancy symptoms.
A note from Motherly
Going through an ectopic pregnancy can be stressful or traumatizing, just as with any pregnancy loss. Be sure to take ample time to work through your feelings, talk to a counselor and join online support groups with other people who’ve gone through ectopic pregnancies to for added support.
Sources
Chukus A, Tirada N, Restrepo R, and Reddy NI. Uncommon implantation sites of ectopic pregnancy: Thinking beyond the Complex Adnexal Mass. RadioGraphics 2015 35:3, 946-959. doi:10.1148/rg.2015140202
Lozeau AM, Potter B. Diagnosis and management of ectopic pregnancy. Am Fam Physician. 2005 Nov 1;72(9):1707-14. Erratum in: Am Fam Physician. 2007 Feb 1;75(3):312.
Seeber, Beata E. MD1; Barnhart, Kurt T. MD, MSCE1,2 Suspected Ectopic Pregnancy. Obstetrics & Gynecology: February 2006 – Volume 107 – Issue 2 Part 1 – p 399-413. doi:10.1097/01.AOG.0000198632.15229.be
Zachariah SK, Fenn M, Jacob K, Arthungal SA, Zachariah SA. Management of acute abdomen in pregnancy: current perspectives. Int J Womens Health. 2019 Feb 8;11:119-134. doi:10.2147/IJWH.S151501