I recently noticed something very odd, something very different about this pregnancy. Over 30 weeks in, and I’ve yet to receive a single solicitation from the cord blood banks. Last time, the emails came at least weekly. Then daily. Then the phone calls started. Offers of free information kits, sweepstakes drawings, $100 off the collection fee, before-you-hang-up-here’s-my-supervisor-with-an-even-better-offer high pressure sales calls.

This time, nothing, save for a half-hearted offer of a brochure at a maternity store.
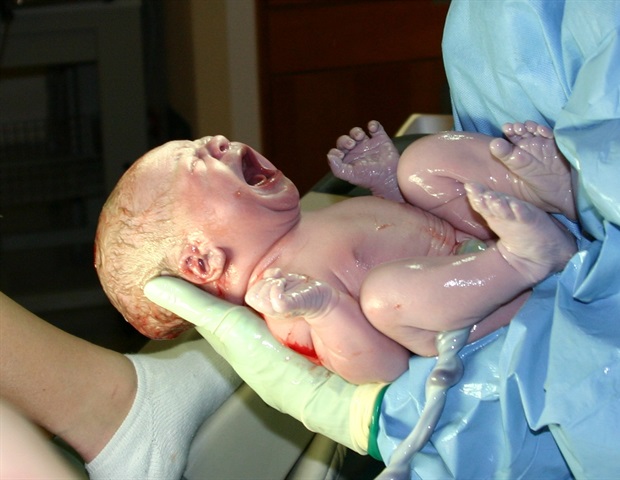
Cord blood banking, as the name suggests, involves the collection and storage of your newborn’s umbilical cord blood. Tasty, delicious, stem-cell-rich cord blood. These unformed stem cells have the ability to turn into mature blood cells — and could save the life of someone who needs a bone marrow transplant, and possibly other diseases, since stem-cell research remains in its infancy, really. Three years ago, it was heralded as the greatest life insurance policy you could buy for your child and family.
Of course, this policy comes with a steep price tag — anywhere from $1,000 to $2,000 for the initial collection, plus a yearly storage fee of at least $100, plus other additional fees that can quickly add up. While many new parents are horrified at the idea of letting a little thing like TWO THOUSAND DOLLARS affect a decision that could SAVE THEIR BABY’S LIFE, it is a lot of money. Let’s put on our calm, rational thinking caps here.
1) Cord-blood banking is generally only recommended for families with a known history of certain diseases, or who already have a relative suffering from such a disease who could benefit from the cells. These diseases include leukemia or lymphoma, aplastic anemia, severe sickle cell anemia, and severe combined immune deficiency. It’s nice to dream about a future where stem cells will be able to wipe out pretty much any disease known to man, but for now, that’s the list.
2) The odds that your baby will actually be able to use his or her own umbilical cord blood are low. Again, this is tempered by the relative “newness” of cord blood banking and transplants, but for now the statistics just don’t exist for patients receiving their own cord blood to prove that it’s better, safer or at all effective. (Some experts point out that a sick baby who receives his or her own stem cells during a transplant could very well just develop the disease all over again.)
3) Stem-cell transplants are generally only done on children and teenagers, since the amount collected at birth is simply too small for most adult transplants. (The larger the person, the more cells are needed for an effective transplant.) C-section deliveries generally yield an even smaller number of usable cells, since the collection usually can’t happen until after the mother’s uterus has been sewn up. If your family has a history of childhood cancers or an older sibling needs a bone marrow transplant, cord-blood collection may be a no-brainer. But parents who are being pitched on banking as a lifelong investment in bionic super health (stem cells can, theoretically, be stored forever) need to know that the window of actual usability is limited by the patient’s age.
4) Another unknown (for now, anyway) is whether or not a cord blood donation from a relative is any better or more effective than one from an unrelated donor, which happens successfully all the time. Stem cells are truly “blank” cells; highly adaptable and at low risk for rejection. Unlike organ transplants, there’s no need for a “perfect” stem cell match for a successful transplant.
5) That said, parents of racially or ethnically diverse children may want to bank cord blood because it IS statistically harder to find a bone marrow match in these cases. The National Marrow Donor Program specifically encourages cord blood donations from the following communities, where there is often a critical shortage of matching marrow donors:
Black and African American
American Indian and Alaska Native
Asian
Native Hawaiian and other Pacific Islander
Hispanic and Latino
Multiple race
Donating Cord Blood
And on that note, what about donating your baby’s cord blood? Why, sure! And become a marrow donor yourself, while you’re at it. (It’s easy and painless, done with a single swab of your cheek, full details here.) The full and extensive list of FAQs for cord blood donation can be found here.
It’s important to read and process them all — it’s best to set up your donation by the 34th week of pregnancy, donations from twins and multiples are not accepted, and only about 50% of donations can actually be stored for transplantation because cord blood units do yield such small amounts. However, while the American Academy of Pediatrics believes “storing cord blood as ‘biological insurance’ should be discouraged because there currently is no scientific data to support (self) autologous transplantation,” they DO encourage donating the blood to public banks, both for transplants and research purposes. And no, it costs you nothing to donate your baby’s cord blood, other than a few phone calls to make arrangements before you give birth.

























































![What Really Happens If You Drop A Penny From The Top Of The Empire State Building? [Video]](https://kidsactivitiesblog.com/wp-content/uploads/2016/08/When-you-drop-a-penny-from-the-empire-state-building-video-Kids-Activities-Blog-fb.png)











_-_Ekaterina_Markelova_M2_4392c2cb09c3463c87360cc051af7033-620x480.jpg)


